Results
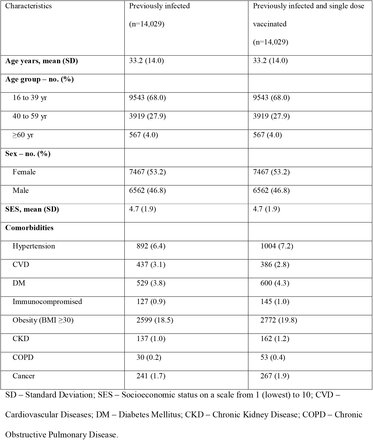
Overall, 673,676 MHS members 16 years and older were eligible for the study group of fully vaccinated SARS-CoV-2-naïve individuals; 62,883 were eligible for the study group of unvaccinated previously infected individuals and 42,099 individuals were eligible for the study group of previously infected and single-dose vaccinees.
Model 1 – previously infected vs. vaccinated individuals, with matching for time of first event
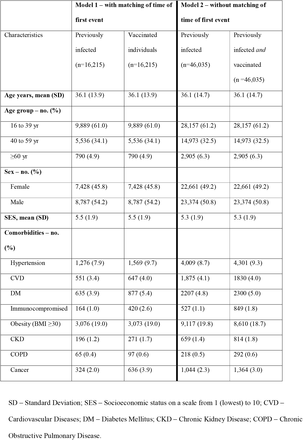
In model 1, we matched 16,215 persons in each group. Overall, demographic characteristics were similar between the groups, with some differences in their comorbidity profile (
Table 1a).
During the follow-up period, 257 cases of SARS-CoV-2 infection were recorded, of which 238 occurred in the vaccinated group (breakthrough infections) and 19 in the previously infected group (reinfections). After adjusting for comorbidities, we found a statistically significant 13.06-fold (95% CI, 8.08 to 21.11) increased risk for breakthrough infection as opposed to reinfection (
P<0.001). Apart from age ≥60 years, there was no statistical evidence that any of the assessed comorbidities significantly affected the risk of an infection during the follow-up period (
Table 2a). As for symptomatic SARS-COV-2 infections during the follow-up period, 199 cases were recorded, 191 of which were in the vaccinated group and 8 in the previously infected group. Symptoms for all analyses were recorded in the central database within 5 days of the positive RT-PCR test for 90% of the patients, and included chiefly fever, cough, breathing difficulties, diarrhea, loss of taste or smell, myalgia, weakness, headache and sore throat.
After adjusting for comorbidities, we found a 27.02-fold risk (95% CI, 12.7 to 57.5) for symptomatic breakthrough infection as opposed to symptomatic reinfection (P<0.001) (Table 2b). None of the covariates were significant, except for age ≥60 years.
Nine cases of COVID-19-related hospitalizations were recorded, 8 of which were in the vaccinated group and 1 in the previously infected group (Table S1). No COVID-19-related deaths were recorded in our cohorts.